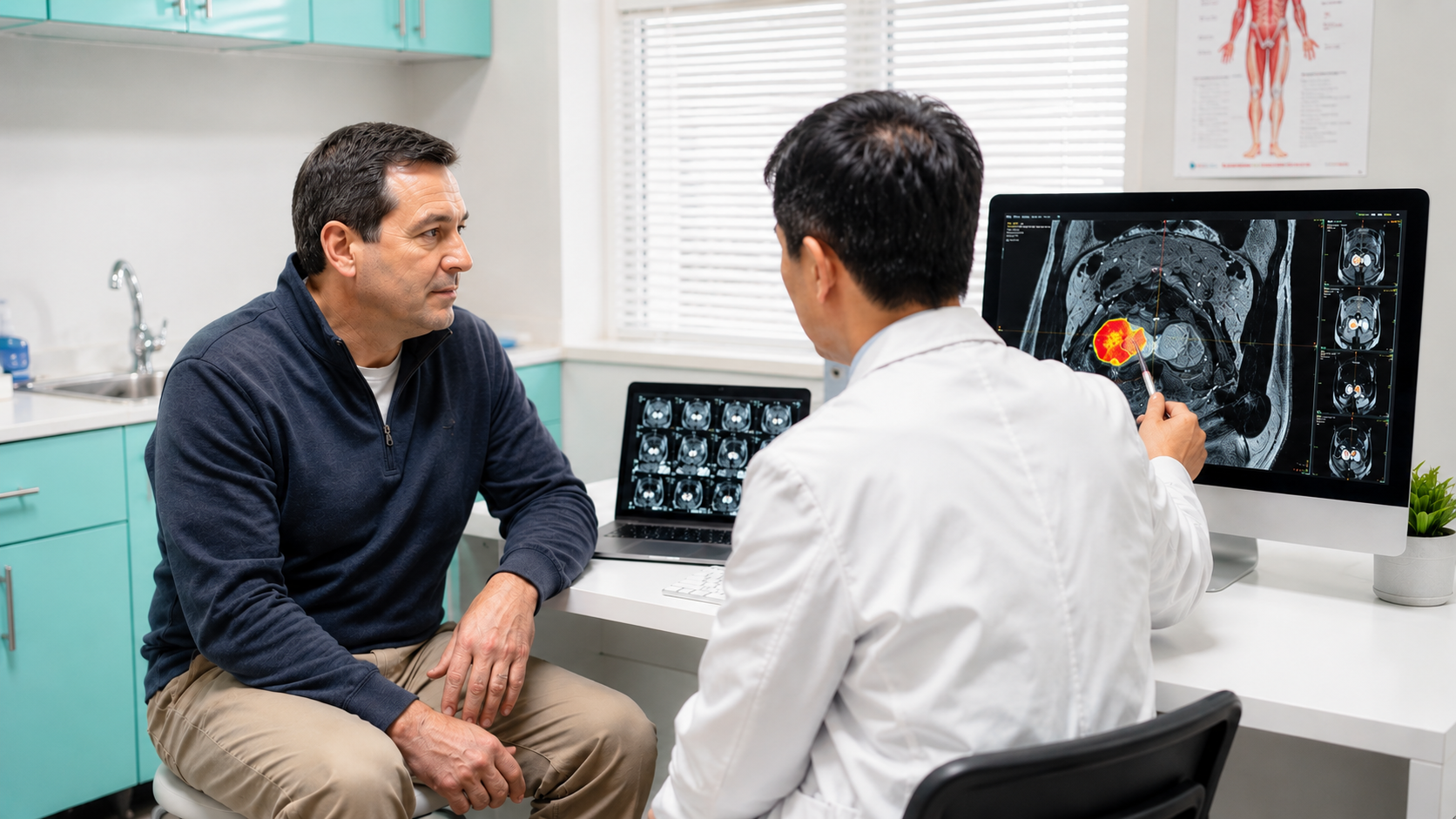
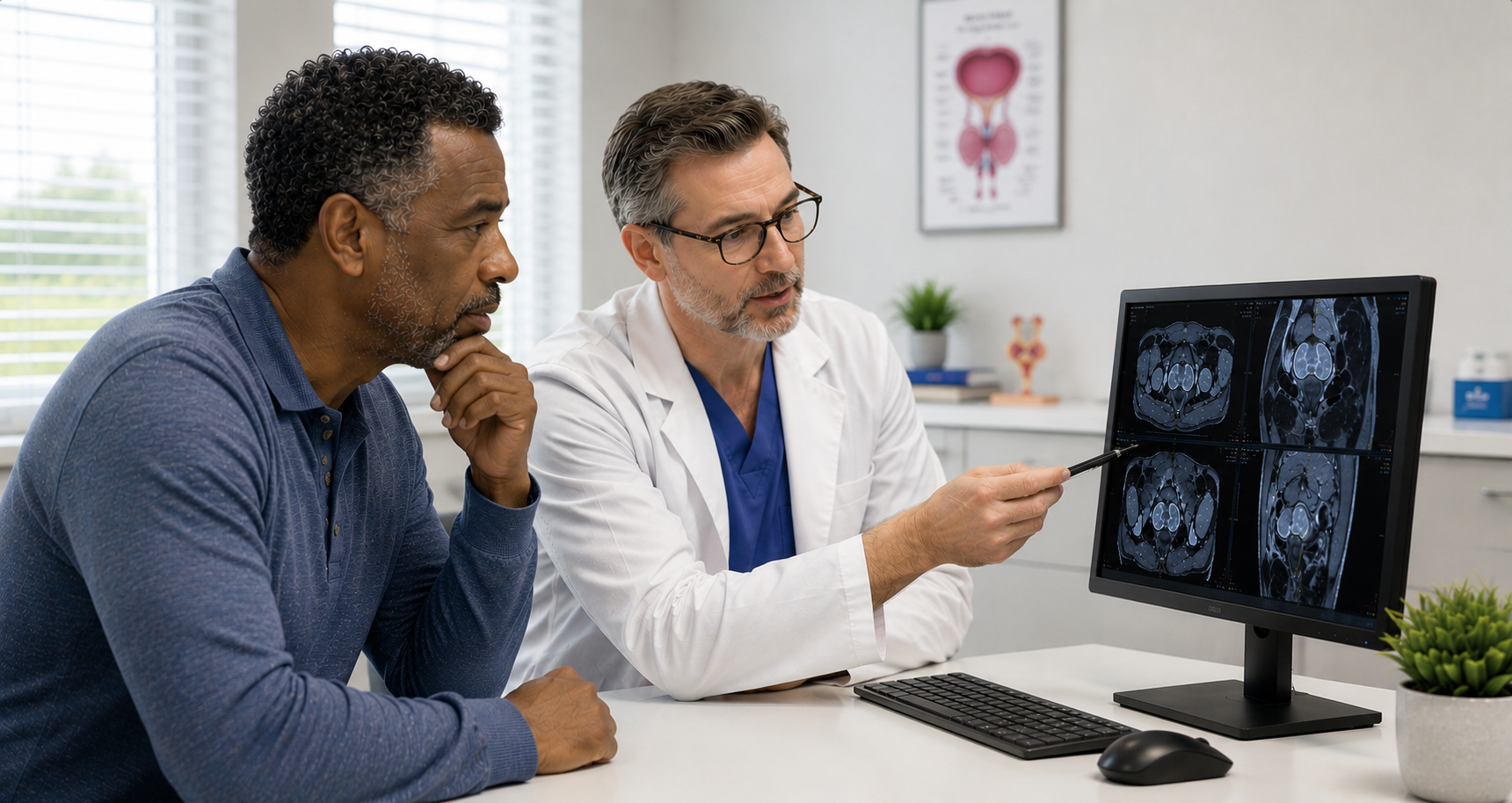
Why Expertise Matters in MRI Interpretation
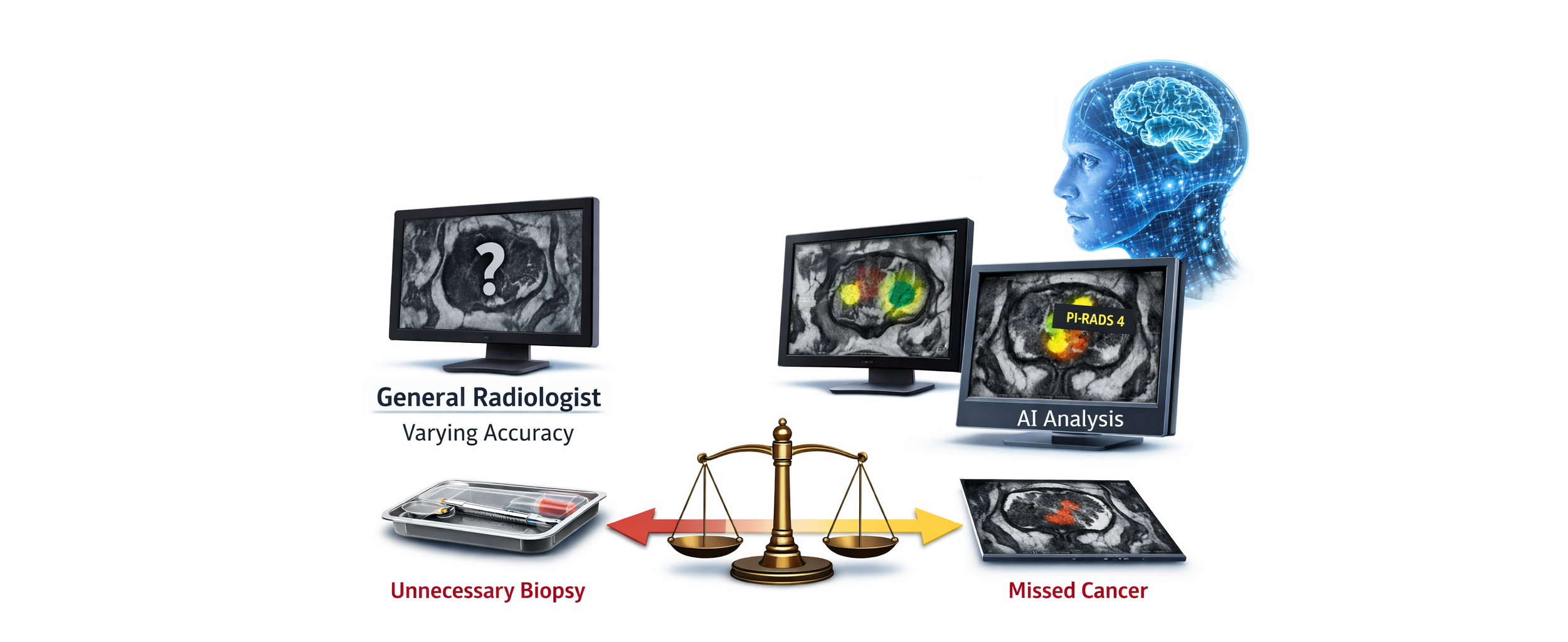
A prostate MRI is only as good as the radiologist who reads it. While MRI technology has revolutionized prostate cancer detection, significant variability exists in how different radiologists interpret the same images. Understanding this "reader gap" helps explain why expert interpretation—and increasingly, AI assistance—can make a meaningful difference in diagnostic accuracy.
The Variability Problem Is Real
Despite PI-RADS providing a structured scoring framework, radiologists frequently disagree on what they see. Across multiple studies, inter-reader agreement for PI-RADS scoring ranges from poor to moderate:
- Kappa values of 0.24 to 0.57 across published studies—meaning radiologists agree on the exact PI-RADS score only about 46–68%of the time.
- A landmark 2017 UK study found that when subspecialist radiologists re-read prostate MRIs originally interpreted at community hospitals, they disagreed with the initial reading in 54% of cases.
- Essentially zero agreement on PI-RADS 3 lesions between community and academic radiologists in a 2024 comparison study.
The most consequential disagreements cluster around PI-RADS 3, the equivocal category that sits precisely at the biopsy decision threshold. Since PI-RADS 3 is where clinicians decide whether to biopsy or monitor, inconsistency here directly translates to real clinical consequences: some men receive unnecessary biopsies while others have dangerous cancers missed.
Research has identified specific areas where radiologist interpretation varies most:
- Transition zone lesions (tumors in the inner portion of the prostate) generate more disagreement than peripheral zone lesions.
- The distinction between moderately and markedly restricted diffusion on DWI—the difference between PI-RADS 3 and 4—remains one of the most subjective calls in prostate imaging.
Small lesions and multifocal disease are more likely to be missed or mischaracterized by less-experienced readers.
The most detailed comparison comes from a 2021 MD Anderson study examining 302 lesions in 194 patients:
- Dedicated prostate MRI radiologists: 85.9%sensitivity and 77.3% specificity
- General abdominal radiologists: 70.7%sensitivity and 46.8% specificity
- Overall accuracy gap: 80.1% versus 54.6%
The general radiologists also dramatically overcalled findings, assigning more than twice as many high-suspicion scores—which would trigger unnecessary biopsies.
Second opinions from subspecialists demonstrably improve outcomes. The 2017 UK second-opinion study showed that expert re-reads:
- Improved negative predictive value from 0.72 to 0.89
- Improved positive predictive value from 0.28 to 0.61
- Paradoxically, experts were more likely to call scans negative (41% vs. 20%), reducing overcalling while catching more true cancers
Both improvements were statistically significant and clinically meaningful.
Consensus panels recommend a minimum of 50–100 cases for basic qualification in prostate MRI interpretation, with 1,000+ cases considered necessary to achieve expert status. Germany has implemented the only national certification program, with over 685 certified radiologists meeting standardized competency requirements.
The challenge is that most community radiology practices do not have dedicated prostate MRI subspecialists, and many radiologists reading prostate MRIs may fall below the volume thresholds associated with expert performance.
Several approaches are emerging to address reader variability:
- Subspecialist second opinions: Sending difficult cases to academic centers or dedicated prostate imaging specialists for re-interpretation.
- AI-assisted interpretation: Using FDA-cleared AI tools that can help less-experienced readers achieve performance closer to expert levels.
- Standardized training and certification: Formal programs to ensure radiologists meet minimum competency standards before interpreting prostate MRIs.
For patients, the takeaway is clear: not all MRI readings are created equal. If you receive a PI-RADS 3 score or if your results seem inconsistent with your clinical picture, seeking a second opinion from a subspecialist or an AI-enhanced analysis may provide valuable additional information.
Sources: UK Second-Opinion Study (2017), MD Anderson Comparison Study (2021), Inter-reader Agreement Meta-analyses, German Certification Program Data